General Findings. Chickenpox is a childhood disease characterized by mild systemic symptoms and a generalized intensely pruritic eruption of maculopapular lesions that rapidly develop into vesicles on an erythematous base. Oral vesicles that rapidly change to ulcers may be seen, but the oral lesions are not an important symptomatic, diagnostic, or management problem.
HZ commonly has a prodromal period of 2 to 4 days, when shooting pain, paresthesia, burning, and tenderness appear along the course of the affected nerve. Unilateral vesicles on an erythematous base then appear in clusters, chiefly along the course of the nerve, giving the characteristic clinical picture of single dermatome involvement. Some lesions spread by viremia occur outside the dermatome. The vesicles turn to scabs in 1 week, and healing takes place in 2 to 3 weeks. The nerves most commonly affected with HZ are C3, T5, L1, L2, and the first division of the trigeminal nerve.
When the full clinical picture of HZ is present with pain and unilateral vesicles, the diagnosis is not difficult. Diagnostic problems arise during the prodromal period, when pain is present without lesions. Unnecessary surgery has been performed because of the diagnosis of acute appendicitis, cholecystitis, or dental pulpitis.
A more difficult diagnostic problem is pain caused by VZ virus without lesions developing along the course of the nerve (zoster sine herpete; zoster sine eruptione). Diagnosis in these cases is based on clinical symptoms and serologic evidence of a rising antibody titer.
HZ may also occasionally affect motor nerves. HZ of the sacral region may cause paralysis of the bladder. The extremities and diaphragm have also been paralyzed during episodes of HZ.
The most common complication of HZ is postherpetic neuralgia, which is defined as pain remaining for over a month after the mucocutaneous lesions have healed, although some clinicians do not use the term postherpetic neuralgia unless the pain has lasted for at least 3 months after the healing of the lesions. The overall incidence of postherpetic neuralgia is 12 to 14%, but the risk increases significantly after the age of 60 years, most likely due to the decline in cell-mediated immunity.
32–34
Immunosuppression does not increase the risk of postherpetic neuralgia.
35
Oral Findings. Herpes zoster involves one of the divisions of the trigeminal nerve in 18 to 20% of cases, but the ophthalmic branch is affected several times more frequently than are the second or third divisions. HZ of the first division can lead to blindness secondary to corneal scarring and should be managed by an ophthalmologist. Facial and intraoral lesions are characteristic of HZ involving the second and third divisions of the trigeminal nerve.
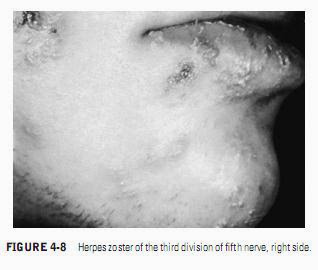
Each individual oral lesion of HZ resembles lesions seen in herpes simplex infections. The diagnosis is based on a history of pain and the unilateral nature and segmental distribution of the lesions (Figures 4-7 and 4-8). When the clinical appearance is typical and vesicles are present, oral HZ can be distinguished clinically from other acute multiple lesions of the mouth, which are bilateral and are not preceded or accom