Histoplasmosis is caused by the fungus Histoplasma capsulatum ,a dimorphic fungus that grows in the yeast form in infected tissue. Infection results from inhaling dust contaminated with droppings, particularly from infected birds or bats. An African form of this infection is caused by a larger yeast, which is considered a variant of H. capsulatum and is called H. duboisii.
Histoplasmosis is the most common systemic fungal infection in the United States; in endemic areas such as the Mississippi and Ohio River valleys, serologic evidence of previous infection may be found in 75 to 80% of the population. In most cases, particularly in otherwise normal children, primary infection is mild, manifesting as a self-limiting pulmonary disease that heals to leave fibrosis and calcification similar to tuberculosis. In a small percentage of cases, progressive disease
results in cavitation of the lung and dissemination of the organism to the liver, spleen, adrenal glands, and meninges. Patients with the disseminated form of the disease may develop anemia and leukopenia secondary to bone marrow involvement. Immunosuppressed or myelosuppressed patients are more likely to develop the severe disseminated form of the disease. During the past decade, most reported cases of oral lesions of histoplasmosis have been reported in HIV-infected individuals who live in or have visited endemic areas.
ORAL MANIFESTATIONS
ORAL MANIFESTATIONS
Oral involvement is usually secondary to pulmonary involvement and occurs in a significant percentage of patients with disseminated histoplasmosis. Oral mucosal lesions may appear as a papule, a nodule, an ulcer, or a vegetation. If a single lesion is left untreated, it progresses from a firm papule to a nodule, which ulcerates and slowly enlarges. The cervical lymph nodes are enlarged and firm. The clinical appearance of the lesions, as well as the accompanying lymphadenopathy, often resembles that of squamous cell carcinoma, other chronic fungal infections, or even Hodgkin’s disease.
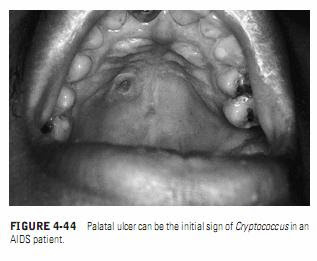
Cases of oral histoplasmosis have been reported as the initial sign of HIV infection. The most common oral lesion of histoplasmosis in patients with HIV is an ulcer with an indurated border, which is most commonly seen on the gingiva, palate, or tongue.These oral histoplasmosis lesions in patients with HIV may occur alone or as part of a disseminated infection.
DIAGNOSIS
DIAGNOSIS
Definitive diagnosis of histoplasmosis is made by a culture of infected tissues or exudates on Sabouraud’s dextrose agar or other appropriate media. Biopsy of infected tissue shows small oval yeasts within macrophages and reticuloendothelial cells as well as chronic granulomas, epithelioid cells, giant cells, and occasionally caseation necrosis. Skin tests and serology are not definitive because of significant numbers of false-negative and false-positive reactions.
TREATMENT
Mild to moderate cases of histoplasmosis can be treated with ketoconazole or itraconazole for 6 to 12 months. Immunosuppressed patients or patients with severe disease require intravenous amphotericin B for up to 10 weeks.
TREATMENT
Mild to moderate cases of histoplasmosis can be treated with ketoconazole or itraconazole for 6 to 12 months. Immunosuppressed patients or patients with severe disease require intravenous amphotericin B for up to 10 weeks.